Pharmakokinetik: Cannabis Stoffwechsel
Das Verständnis der Pharmakokinetik, also wie Ihr Körper medizinisches Cannabis aufnimmt und verarbeitet, ist ein wichtiger Baustein für eine erfolgreiche Therapie. Der therapeutische Effekt von Cannabinoiden ist von den Mustern ihrer Absorption, systemischen Verteilung, Verstoffwechselung und Ausscheidung abhängig.Fragen Sie sich, wie schnell der Cannabis-Stoffwechsel ist? Das Verständnis der Pharmakokinetik von Cannabis, also wie Ihr Körper medizinisches Cannabis aufnimmt und verarbeitet, ist ein wichtiger Baustein für eine erfolgreiche Therapie. Insbesondere der Stoffwechsel der Cannabinoide spielt hier eine entscheidende Rolle.
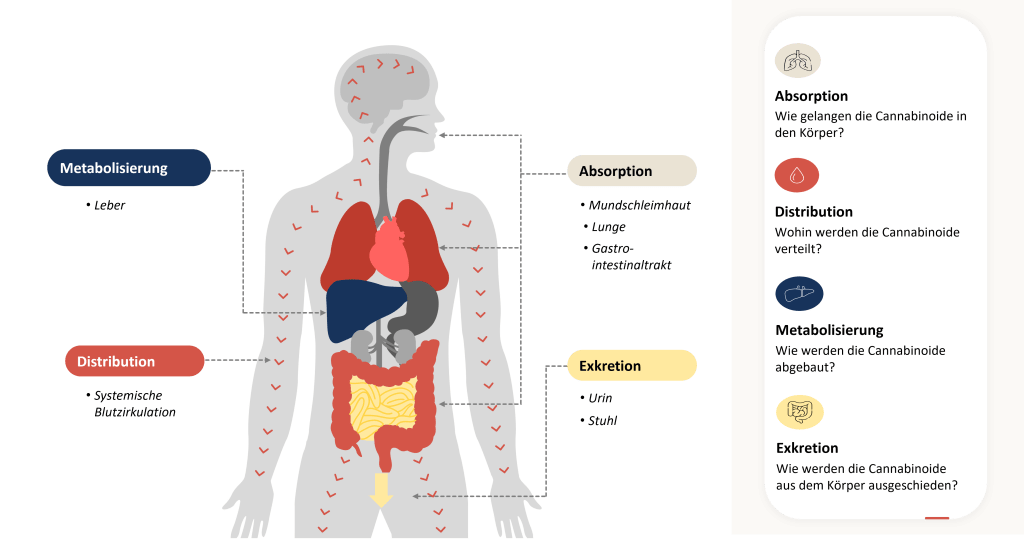
Pharmakokinetik: Wie der Cannabis Stoffwechsel funktioniert
Der therapeutische Effekt von Cannabinoiden ist von den Mustern ihrer Absorption, systemischen Verteilung, Verstoffwechselung und Ausscheidung abhängig. Werden Cannabinoide wie THC als Medikament eingenommen, müssen sie vom Körper absorbiert werden, bevor sie im Körper verteilt, wieder abgebaut (metabolisiert) und ausgeschieden werden. Den gesamten Prozess bezeichnet man als „Pharmakokinetik“. Der Cannabis Stoffwechsel spielt hierbei eine zentrale Rolle. Ihre therapeutische Wirkung entfalten die Cannabinoide nach der Absorption, wenn sie systemisch mit der Blutzirkulation im Körper verteilt werden und unter anderem an die Cannabinoid-Rezeptoren (CB1 und CB2) binden, woraufhin diese aktiviert werden. Die Wirkung der Cannabinoide lässt nach, wenn ihre Konzentration im Blut durch den Abbau und ihre Exkretion (Ausscheidung) mit dem Urin oder Stuhl abnimmt. Eine Ausnahme bildet das erste Abbauprodukt (Metabolit) von THC, das 11-OH-THC, welches ähnliche Wirkungen, wie das THC selbst hat.
Cannabis Stoffwechsel: Welche Rolle spielt die Verabreichungsmethode?
Absorption
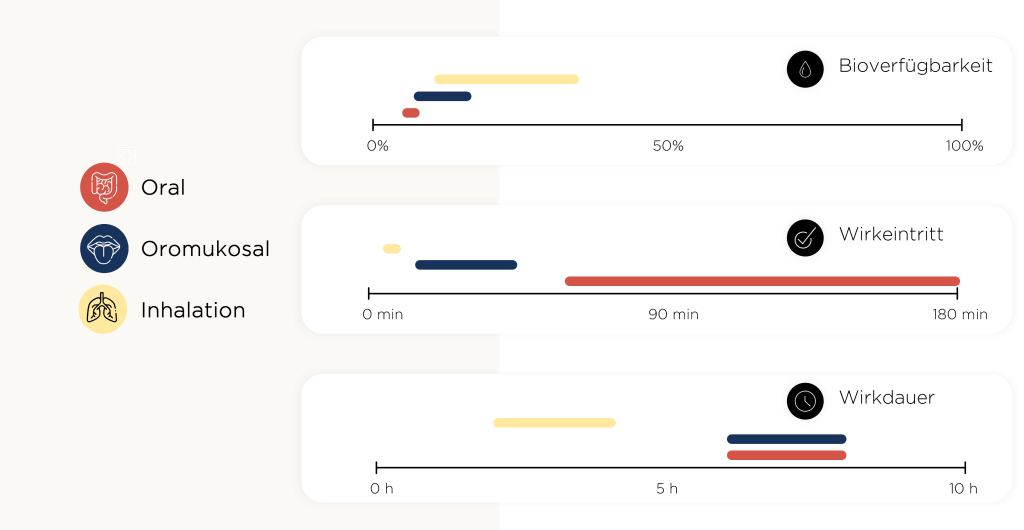
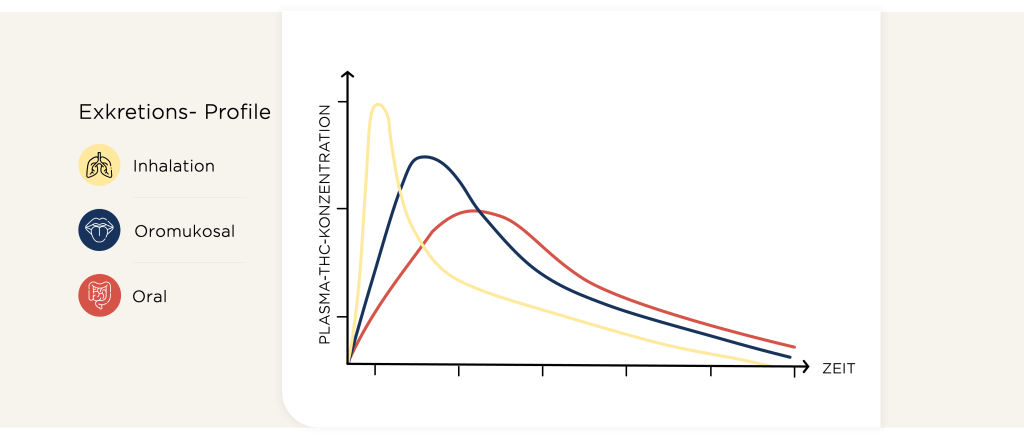
Die Geschwindigkeit und das Ausmaß der Absorption hängen in hohem Maß von der Einnahmeweise des medizinischen Cannabis ab. Die Aufnahme erfolgt üblicherweise peroral (Absorption im Verdauungstrakt nach Schlucken), oromukosal (auf die Mundschleimhaut gesprüht, Absorption ebenfalls größtenteils im Verdauungstrakt), sublingual (unter die Zunge gesprüht, kann je nach Präparat über die Mundschleimhaut aufgenommen werden) oder inhalativ (Aufnahme über die Lungenbläschen). Die schnellste Absorption in den systemischen Blutkreislauf und den schnellsten Wirkeintritt erreicht man durch Inhalation und teils durch sublinguale Präparate (5-10 min), was eine schnelle Linderung von Symptomen und eine schnelle Dosisanpassung ermöglichen kann. Der Wirkeintritt erfolgt bei der oromukosalen und oralen Aufnahme langsamer (45 min -180 min), die Wirkung hält bei sublingualen Präparaten und bei der oralen Gabe länger an, weshalb sich diese Einnahmeweise besonders auch zur Behandlung andauernder Symptome eignet. Die Wirkdauer beträgt bei inhalativer Anwendung etwa 2-4 Stunden, bei oraler, sublingualer und oromukosaler Anwendung etwa 6-8 Stunden¹. Eine Besonderheit stellen neue Formulierungen dar, welche sublingual, also unter die Zunge, eingenommen werden. Hier tritt die Wirkung schon innerhalb von 5-10 Minuten ein und hält trotzdem 6-8 Stunden an. Diese Zeitspannen sind grobe Schätzungen; die tatsächliche Wirkdauer kann von Patient zu Patient unterschiedlich sein. Weitere Faktoren wie zum Beispiel das Wirkstoffdesign, die Nahrungsaufnahme und das Inhalationsmuster können die Absorption beeinflussen.
Distribution (Verteilung)
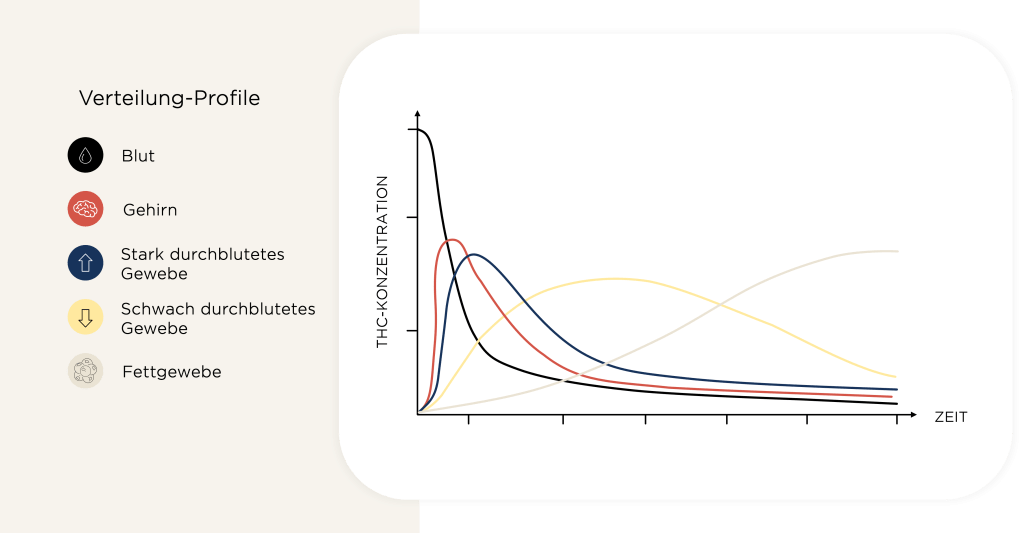
Nach der Absorption erreichen die Wirkstoffe aus der Cannabis-Pflanze zunächst die gut durchbluteten Organe wie Lunge, Herz, Gehirn und Leber. Anschließend erreichen sie das Körperfett, wo sie sich einlagern können und später nach und nach wieder in den Blutkreislauf abgegeben werden können. Faktoren wie Körpergröße, Körperbau und Gesundheitszustand wirken sich auf die Verteilung aus².
Metabolisierung
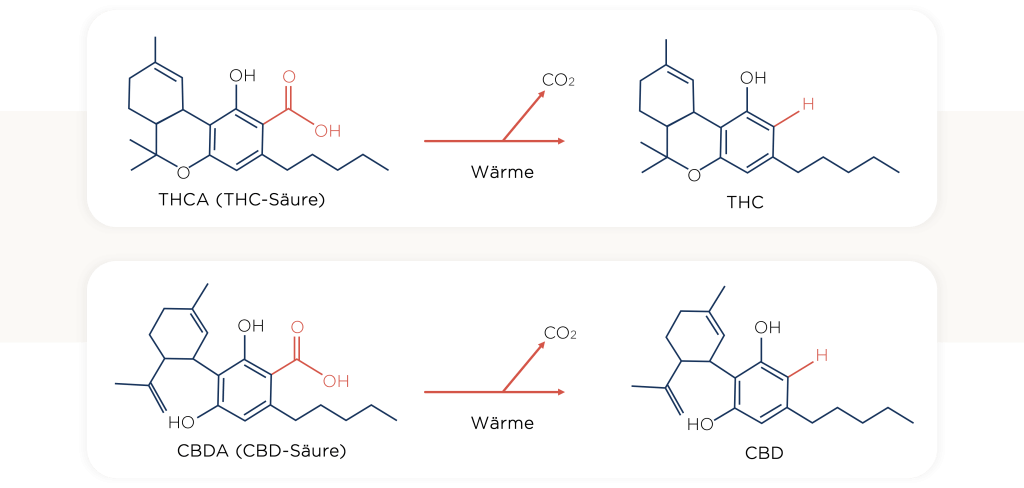
Der Abbau von Cannabinoiden wie THC und CBD erfolgt maßgeblich in der Leber durch CYP450-Enzyme (CYP2C9, CYP2C19, CYP3A4), dabei entstehen sowohl aktive als auch inaktive Metaboliten. THC wird primär in den aktiven und euphorisierend wirkenden Metaboliten 11-OH-THC umgewandelt. Dieser kann weiter zu THC-COOH abgebaut werden³. Die beim Abbau von CBD am häufigsten entstehenden Metaboliten sind die inaktiven 7-COOH und aktiven 7-OH Metaboliten⁴⁻⁶. Bei der oralen Aufnahme von Cannabis liegt die Bioverfügbarkeit (Menge des eingenommenen Wirkstoffs, der die systemische Blutzirkulation erreicht) in manchen Fällen nur bei 6%. Der Grund dafür ist der sogenannte “First-Pass-Effekt”: Oral eingenommene Wirkstoffe werden im Gastrointestinaltrakt absorbiert und erreichen über das Pfortader-System zuerst die Leber – Sowohl im Gastrointestinaltrakt als auch in der Leber werden Teile der Wirkstoffe bereits abgebaut, bevor sie die systemische Blutzirkulation erreichen. Die Bioverfügbarkeit bei inhalativer Anwendung wird auf 10-35% geschätzt. Für die oromukosale Anwendung liegt der Wert zwischen diesen Bereichen. Das liegt wahrscheinlich daran, dass die fettlöslichen Cannabinoide nur zum Teil über die Mundschleimhaut absorbiert werden und ein Teil geschluckt und somit oral aufgenommen wird²,⁷.
Exkretion
Die Ausscheidung der Cannabinoide verläuft bei Patienten in Abhängigkeit von Faktoren wie dem Körperbau, dem Alter, dem allgemeinen Gesundheitszustand usw. unterschiedlich. Die Halbwertszeit (d.h. die Zeitspanne, bis die Blutkonzentration des Wirkstoffs sich halbiert hat) ist zu Beginn sehr kurz und beträgt für THC kurz nach der Einnahme in bestimmten Fällen nur 6 min. Aufgrund der Einlagerung der Cannabinoide ins Körperfett und ihrer von dort aus allmählichen Wiederabgabe in den Blutkreislauf steigt die Halbwertszeit für THC zu späteren Zeitpunkten auf mehr als 22h. Bei wiederholter täglicher Anwendung kann sich die Halbwertszeit sogar auf mehrere Tage verlängern; Cannabinoide sind daher potentiell mehrere Tage nach der Einnahme noch im Blut nachweisbar. Die Bestandteile von Cannabis werden mit dem Stuhl und dem Urin ausgeschieden²,³.
Häufig gestellte Fragen
Was versteht man unter Pharmakokinetik im Zusammenhang mit medizinischem Cannabis?
Die Pharmakokinetik beschreibt, wie medizinisches Cannabis vom Körper aufgenommen (Absorption), verteilt (Distribution), abgebaut (Metabolisierung) und ausgeschieden (Exkretion) wird. Sie bestimmt, wie schnell und wie lange die Wirkung einsetzt1,2.
Welche Rolle spielt die Verabreichungsform bei der Wirkung von medizinischem Cannabis?
Die Aufnahmegeschwindigkeit und Wirkung von Cannabis hängen stark von der Verabreichungsform ab. Inhalative Einnahme wirkt schnell (5–10 Minuten), orale Aufnahme braucht länger (60–180 Minuten), hält aber meist länger an1,2.
Wie schnell wirkt medizinisches Cannabis nach der Einnahme?
Nach inhalativer Einnahme tritt die Wirkung meist innerhalb von 5–10 Minuten ein. Bei oraler oder oromukosaler Einnahme dauert es 15–180 Minuten, bis die Wirkung einsetzt1,2.
Was ist der Unterschied zwischen oraler, inhalativer, oromukosaler und sublingualer Aufnahme von Cannabis?
Inhalative (z.B. Verdampfen) und sublinguale Einnahme können am schnellsten wirken. Inhalation wirkt verhältnismäßig kurz. Orale Einnahme (z. B. Kapseln, Öle) benötigt länger bis zum Wirkungseintritt, die Wirkung hält jedoch, wie bei der sublingualen Gabe, länger an. Nach oromukosale Einnahme (über die Mundschleimhaut) ist der Wirkeintritt nach etwa 45 min, die Wirkdauer ist vergleichbar mit oraler und sublingualer Gabe.1,2,3.
Wie verteilt sich medizinisches Cannabis nach der Aufnahme im Körper?
Nach der Absorption wird Cannabis zunächst in gut durchblutete Organe wie Gehirn, Herz, Lunge und Leber transportiert. Anschließend lagert es sich im Körperfett ein und wird langsam wieder ins Blut abgegeben2.
Was bedeutet Bioverfügbarkeit bei medizinischem Cannabis?
Bioverfügbarkeit beschreibt, wie viel des Wirkstoffs tatsächlich im Blutkreislauf ankommt. Bei oraler Aufnahme liegt sie oft nur bei 6 %, bei inhalativer Aufnahme bei 10–35 %, da bei oraler Einnahme ein Großteil im Verdauungstrakt und in der Leber abgebaut wird („First-Pass-Effekt“)1,2.
Wie werden THC und CBD im Körper abgebaut?
THC und CBD werden vor allem in der Leber durch CYP450-Enzyme abgebaut. THC wird in den aktiven Metaboliten 11-OH-THC und weiter zu THC-COOH umgewandelt, CBD zu verschiedenen inaktiven und aktiven Metaboliten3,4,5.
Was ist der „First-Pass-Effekt“ bei oraler Einnahme?
Beim First-Pass-Effekt werden Wirkstoffe bei der oralen Einnahme im Darm und vor allem in der Leber abgebaut, bevor sie in den systemischen Kreislauf gelangen. Dadurch ist die Bioverfügbarkeit niedriger2,7.
Wie lange hält die Wirkung von medizinischem Cannabis an?
Die Wirkdauer hängt von der Aufnahmeform ab: Inhalativ 2–4 Stunden, oral oder oromukosal 6–8 Stunden. Bei sublingualer Anwendung kann die Wirkung schon nach 5–10 Minuten eintreten und ebenfalls 6–8 Stunden anhalten1.
Wie werden Cannabinoide aus dem Körper ausgeschieden?
Cannabinoide werden vor allem mit dem Stuhl und Urin ausgeschieden. Die Halbwertszeit variiert je nach Körperfett, Einnahmeform und individuellen Faktoren2,3.
Was ist die Halbwertszeit von THC und CBD?
Unmittelbar nach der Einnahme beträgt die Halbwertszeit von THC etwa 6 Minuten. Aufgrund der Einlagerung ins Fettgewebe kann sie später auf über 22 Stunden steigen. Bei regelmäßiger Anwendung sind Cannabinoide noch Tage nach der Einnahme im Blut nachweisbar3,7.
Warum können Cannabinoide Tage nach der Einnahme noch im Blut nachweisbar sein?
Weil sich Cannabinoide im Körperfett einlagern und dort gespeichert werden. Sie werden langsam wieder ins Blut abgegeben und ausgeschieden, weshalb sie auch noch Tage später nachweisbar sind2,3.
Wie beeinflussen Körperbau und Gesundheitszustand die Pharmakokinetik von Cannabis?
Faktoren wie Körpergewicht, Körperfettanteil, Alter und Gesundheitszustand beeinflussen, wie schnell und wie lange Cannabinoide wirken und wie sie im Körper gespeichert oder abgebaut werden2,3.
Welche aktiven und inaktiven Metaboliten entstehen beim Abbau von THC und CBD?
Beim Abbau von THC entsteht der aktive Metabolit 11-OH-THC und der inaktive THC-COOH. Bei CBD entstehen die inaktiven 7-COOH- und die aktiven 7-OH-Metaboliten3,4,5,6.
Welche Rolle spielen CYP450-Enzyme beim Cannabis-Stoffwechsel?
CYP450-Enzyme in der Leber (u. a. CYP2C9, CYP2C19, CYP3A4) sind maßgeblich für den Abbau von THC und CBD verantwortlich und beeinflussen so Wirkdauer und Wirkung2,4,5.
Wie unterscheiden sich die Wirkungsdauer und der Wirkungseintritt bei verschiedenen Einnahmearten?
Inhalativ wirkt Cannabis nach 5–10 Minuten, oral nach 60–180 Minuten. Inhalativ hält die Wirkung 2–4 Stunden an, oral oder oromukosal meist 6–8 Stunden. Sublingualer Konsum bietet schnellen Wirkungseintritt und lange Wirkungsdauer1,2.
Welche Faktoren beeinflussen die Wirkung von medizinischem Cannabis?
Neben Einnahmeform und Dosierung beeinflussen auch Inhalationsmuster, Nahrungsaufnahme, Körperfettanteil, individuelle Enzymaktivität und Begleitmedikation die Wirkung von medizinischem Cannabis1,2,4.
Was ist der Unterschied zwischen systemischer Verteilung und Einlagerung im Körperfett?
Systemische Verteilung bedeutet, dass die Cannabinoide mit dem Blut in Organe gelangen. Im Körperfett werden sie gespeichert und langsam wieder ins Blut abgegeben, was die Nachweisbarkeit verlängert2.
Können Medikamente die Pharmakokinetik von Cannabis beeinflussen?
Ja, insbesondere Medikamente, die die Aktivität von CYP450-Enzymen verändern, können den Abbau von THC und CBD beeinflussen und damit Wirkung und Nebenwirkungen verändern4,5.
Welche wissenschaftlichen Quellen gibt es zur Pharmakokinetik von Cannabinoiden?
Wissenschaftliche Übersichten finden Sie beispielsweise bei MacCallum & Russo (2018), Lucas et al. (2018), Grotenhermen (2003) oder Heuberger et al. (2015)1,2,3,7.
Quellenangaben
- MacCallum, C. A. & Russo, E. B. Practical considerations in medical cannabis administration and dosing. European Journal of Internal Medicine vol. 49 12–19 (2018).
- Lucas, C. J., Galettis, P. & Schneider, J. The pharmacokinetics and the pharmacodynamics of cannabinoids. British Journal of Clinical Pharmacology vol. 84 2477–2482 (2018).
- Heuberger, J. A. A. C. et al. Population Pharmacokinetic Model of THC Integrates Oral, Intravenous, and Pulmonary Dosing and Characterizes Short- and Long-term Pharmacokinetics. Clinical Pharmacokinetics 54, 209–219 (2015).
- Landmark, C. J. & Brandl, U. Pharmacology and drug interactions of cannabinoids. Epileptic Disorders 22, S16–S22 (2020).
- Taylor, L., Gidal, B., Blakey, G., Tayo, B. & Morrison, G. A Phase I, Randomized, Double-Blind, Placebo-Controlled, Single Ascending Dose, Multiple Dose, and Food Effect Trial of the Safety, Tolerability and Pharmacokinetics of Highly Purified Cannabidiol in Healthy Subjects. CNS Drugs 32, 1053–1067 (2018).
- Ujváry, I. & Hanuš, L. Human Metabolites of Cannabidiol: A Review on Their Formation, Biological Activity, and Relevance in Therapy. Cannabis and Cannabinoid Research vol. 1 90–101 (2016).
- Grotenhermen, F. Pharmacokinetics and pharmacodynamics of cannabinoids. Clinical Pharmacokinetics vol. 42 327–360 (2003).
- Ashton, C. H. Pharmacology and effects of cannabis: A brief review. The British Journal of Psychiatry 178, 101–106 (2001).





